Care Within Reach: How Nurse Counsellors Keep You In Good Health
The Primary Care Network (PCN) is a team of healthcare professionals, which comprises of General Practitioners (GPs), Nurse Counsellors, and Care Coordinators, who provide step-by-step care for patients with chronic conditions.
In this installment of “You Ask, We Answer”, let Crystal Lee May May, Assistant Nurse Clinician of I-CARE Primary Care Network, share with you what it's like being a Nurse Counsellor, and how nurse counselling can help you manage your health conditions better.

Ms Crystal Lee May May
Assistant Nurse Clinician, I-CARE Primary Care Network
"1. What does a nurse counsellor do, and who needs their service?"
 Answer:
Answer:
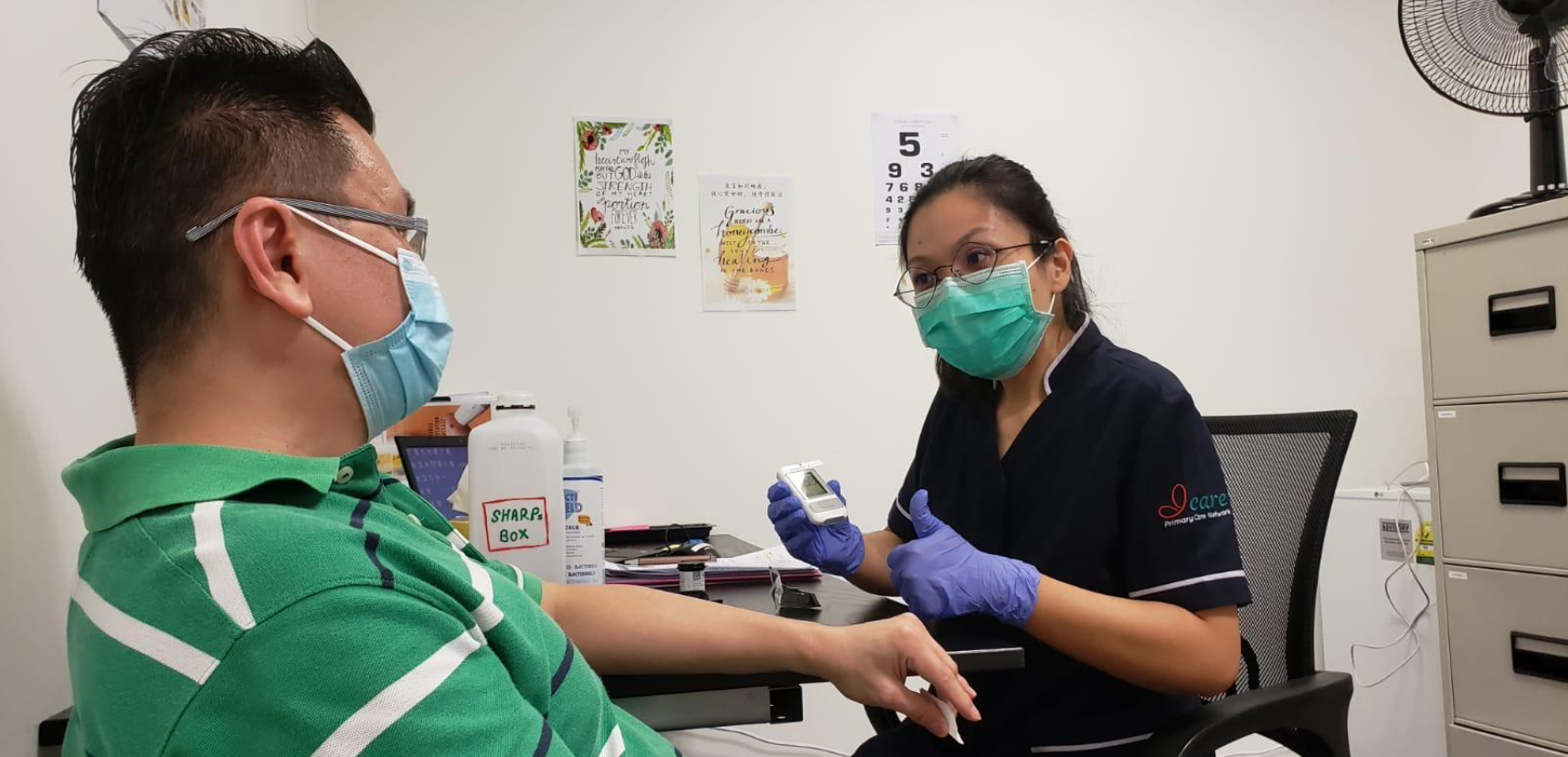
PCN Nurse Counsellors conduct health screenings for patients with chronic health conditions such as Diabetes, Hypertension, Hyperlipidemia, Asthma and/or Chronic Obstructive Pulmonary Disease. These patients are usually referred by PCN GPs.
We also provide nurse counselling, which covers a wide range of topics, including lifestyle modification, to better help patients manage medical conditions. We work closely with our patients to help them make healthier diet choices, introduce exercise regimes into their daily routines, and manage their medications.
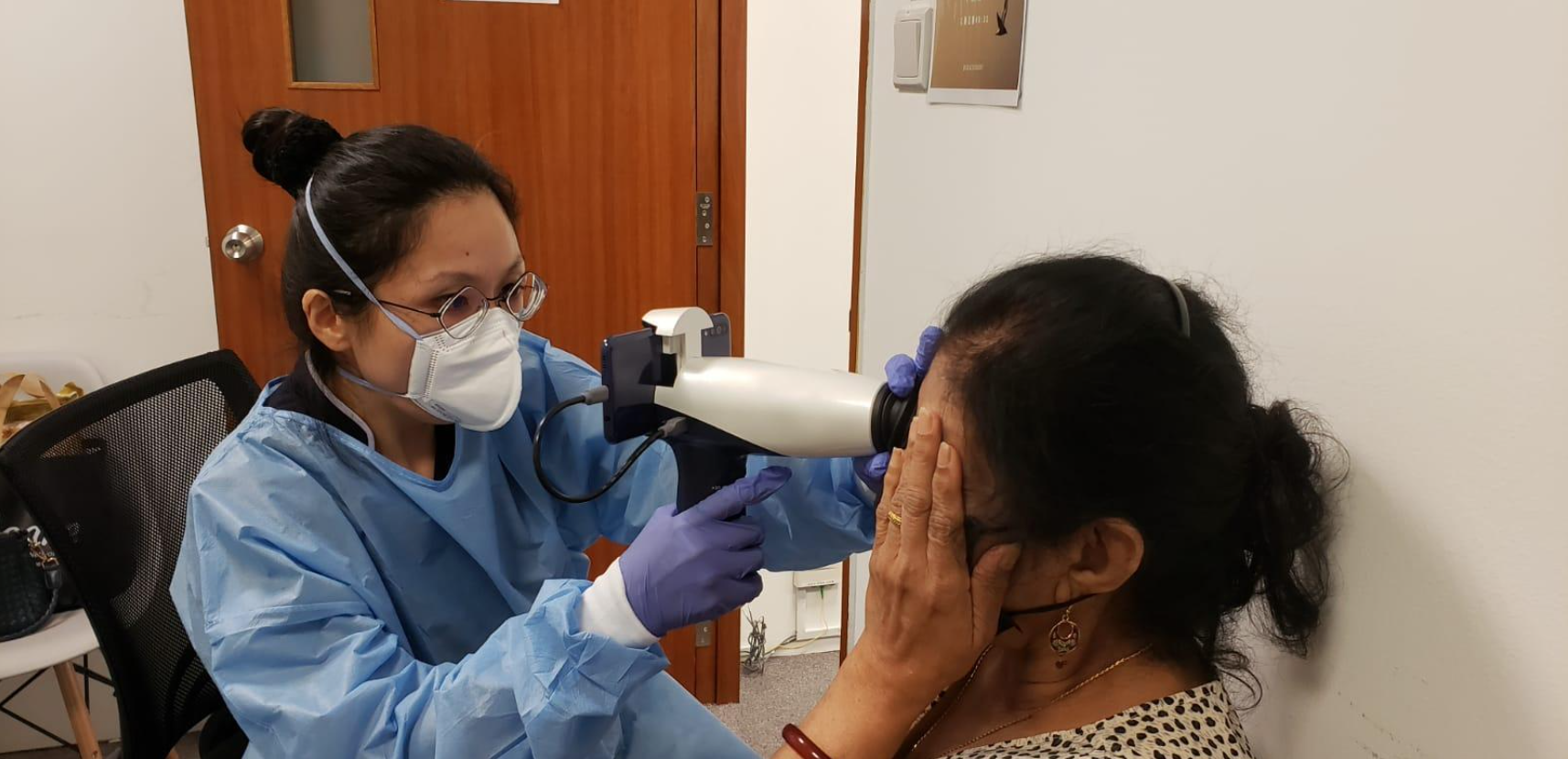
Lastly, we work together with GPs to help patients better manage their disease and have a better quality of life. For example, when GPs start insulin therapy for patients, we provide support by teaching patients and their caregivers insulin injection techniques, equipping them with the self-care management knowledge and skills to better manage their conditions and emotions.
"2. Can you share with us what the process is like from the moment you get a new patient to care for? How often do you check in with the patient?"
 Answer:
Answer:
First, I will get to know our patient’s medical, social, and lifestyle history as this assessment is vital to start a patient-nurse relationship. With this information, a care plan is customised for the patients to tackle their obstacles to achieving a better quality of life. Subsequently, we will discuss the need for nurse counselling.
The frequency of our check-ins with patients depends on a few factors like the type of services the patient is getting, their overall health status, their financial and social conditions, and their suitability for virtual counselling sessions.
"3. How does nurse counselling benefit PCN patients?"
 Answer:
Answer:
We work closely with GPs to provide customised holistic care to our PCN patients. Patients get direct and personal interaction with Nurse Counsellors through counselling sessions. With that, they can clarify any misconceptions about their health conditions and improve their knowledge of self-care management.
"4. Will the GP let patients/caregivers know if they are eligible for PCN services? How else can a patient/caregiver know?"
 Answer:
Answer:
Yes, most of our referrals for PCN services are initiated by GPs. Nurse counsellors, Primary Care Coordinators, and trained health professionals, who help manage a patient's care, could also explain to patients and caregivers the need for PCN services and their eligibility, especially the cost of our services after government subsidies.
"5. What is the difference between nurse counselling and psychological counselling?"
 Answer:
Answer:
The only clear difference is that Nurse Counsellors need to share more about a patients’ chronic disease process and complications.
We help patients recognise their barriers to a better quality of life and arm them with self-care management knowledge and skills. The process allows us to set goals with our patients to manage their chronic conditions sustainably. As in most psychological counselling, we also listen to our patients and affirm their efforts.
"6. How long do you care for each patient? Since your patients’ conditions are chronic, when do they stop needing your services?"
 Answer:
Answer:
As long as the patient continues to see their PCN GP, we will continue to see the patient. The frequency of the follow-up may change depending on the patient’s health condition, financial status and so forth.
We stop seeing the patients when:
- We detect health-related complications that require a referral to specialists in the hospital. The patient will then follow up with the specialists in the hospital.
- The patient moves residence and decides to change to a GP who may not be under the same PCN or is not part of any network. The patient’s health screening may then be carried out in a new PCN or another medical institution.
"7. Why would you recommend for people eligible to go for PCN GPs? How can it benefit them as compared to regular GPs?"
 Answer:
Answer:
Visiting a PCN GP is especially beneficial for patients with chronic health conditions. A PCN GP can tap on the available resources of Nurse Counsellors to provide in-house nursing services that are otherwise available only at the bigger healthcare establishments. These services are reasonably priced, with government subsidies, and not always more expensive than the public institutions.
Beyond resources, PCN GPs also have these benefits:
- Nursing services are often brought into our PCN clinics, making them accessible for our patients who work or live near the clinic.
- Primary Care Coordinators and Nurse Counsellors complement the PCN GPs by keeping track of the patients’ appointment dates and ensuring timely intervention when needed.
"8. Can you share some tips for caregivers who are caring for loved ones with chronic conditions? Anything they can do at home to help their loved ones?"
 Answer:
Answer:
The caregiving journey may be draining for both patients and caregivers physically, emotionally and mentally.
Caregivers should take part during the nurse counselling sessions. We always try to involve the patient’s family member or caregiver when we meet our patients to work towards a shared understanding and goal.
Caregivers should also learn to recognise the patient’s medical signs and symptoms, disease management and coping strategies to take care of both the patient and their personal well-being.
Caregivers and patients should be seen as one unit to achieve a better quality of life. Nurse Counsellors are able to recommend community resources and other support for the caregiver and patient where help is needed.


